 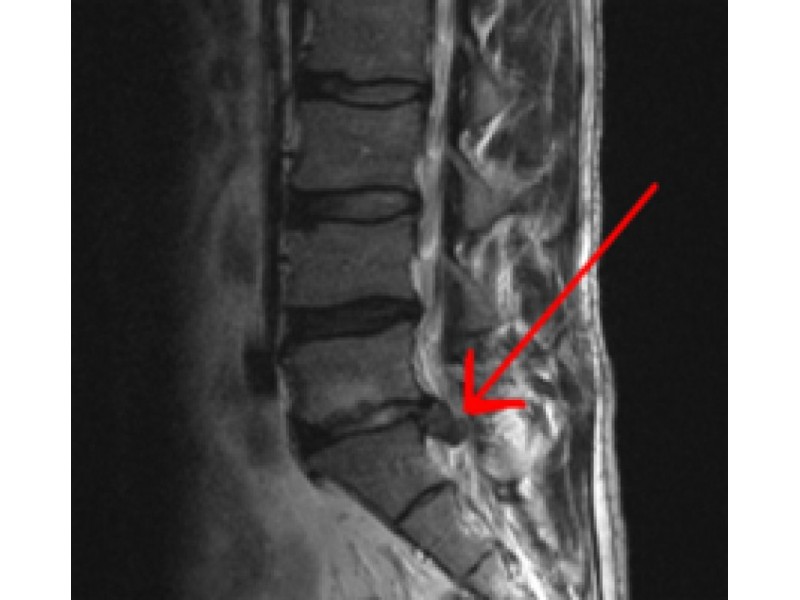
Radiographic imaging, such as an MRI, is not recommended by the American College of Radiology, unless symptoms have been present for six weeks.Primary care evaluation during this time may lead to considering other non-surgical treatments noted below, such as physical therapy.Walking as tolerated is encouraged, along with an anti-inflammatory, such as ibuprofen, if not contraindicated for the patient. The time to improve varies, ranging from a few days to a few weeks. With time, the symptoms of sciatica/radiculopathy improve in approximately 9 out of 10 people. The pain may increase with certain positions or movements of the neck.įortunately, the majority of herniated discs do not require surgery. Along with leg pain, one may experience low back pain however, for acute sciatica the pain in the leg is often worse than the pain in the low back.Ĭervical spine (neck): Cervical radiculopathy is the symptoms of nerve compression in the neck, which may include dull or sharp pain in the neck or between the shoulder blades, pain that radiates down the arm to the hand or fingers or numbness or tingling in the shoulder or arm. 
Straightening the leg on the affected side can often make the pain worse. It may be more severe with standing, walking or sitting. This pain often is described as sharp and electric shock-like. Usually, one side (left or right) is affected. Pressure on one or several nerves that contribute to the sciatic nerve can cause pain, burning, tingling and numbness that radiates from the buttock into the leg and sometimes into the foot. Lumbar spine (lower back): Sciatica/Radiculopathy frequently results from a herniated disc in the lower back. Typically, a herniated disc is preceded by an episode of low back pain or a long history of intermittent episodes of low back pain. If it is pressing on a nerve, there may be pain, numbness or weakness in the area of the body to which the nerve travels. If the herniated disc is not pressing on a nerve, the patient may experience a low backache or no pain at all. Symptoms vary greatly, depending on the position of the herniated disc and the size of the herniation. The area in which pain is experienced depends on what part of the spine is affected. Herniated discs are more common in the lower back (lumbar spine), but also occur in the neck (cervical spine). Herniated discs can occur in any part of the spine. Due to this displacement, the disc presses on spinal nerves, often producing pain, which may be severe. The spinal canal has limited space, which is inadequate for the spinal nerve and the displaced herniated disc fragment. 
Discs that become herniated usually are in an early stage of degeneration. Located between each of the vertebra in the spinal column, discs act as shock absorbers for the spinal bones.Ī herniated disc (also called bulged, slipped or ruptured) is a fragment of the disc nucleus that is pushed out of the annulus, into the spinal canal through a tear or rupture in the annulus. These discs are round, like small pillows, with a tough, outer layer (annulus) that surrounds the nucleus. The bones (vertebrae) that form the spine in the back are cushioned by discs. Herniated Disc | American Association of Neurological Surgeons 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
